“She’s gone.”
Those were the words spoken by the head ICU doctor at NYU Langone at 2:01pm on September 19th, 2018 after listening for Sally’s heartbeat for over a full minute. There was no heartbeat, we had lost her.
We did everything we could.
The doctors, nurses and medical staff did everything they could.
It wasn’t enough, our baby girl’s body was just too weak from cancer treatment and the lingering effects to fight off whatever unforgiving infection had entered her body.
This is the blog post I never wanted to have to write, especially just six years into Sally’s life. We needed more time. More time to spend with our little girl dancing, snuggling, laughing. More time for doctors and nurses to figure out what was occurring in Sally’s body. I wrote the following in our last blog post just two months ago, it haunts me to go back and see these prophetic words:
“…it feels like we’re just fighting to keep Sally alive every day, hoping it buys her time for somebody to figure out how to help her before it’s too late.”
It was too late. We had run out of time. Instead, I’m sitting here writing from Sally’s room laying on her bed, a lock of her golden hair resting next to me where she slept, trying to find the words to explain what happened. I’m in here because I needed to feel close to her as I wrote, I needed her strength to get me through this. As I’m just about to sit down to start writing, the theme song from the Curious George movie, one of her favorites, just came on. Now I know she’s here with me. Thank you Sunshine, we’ll do this “together” as you always loved to tell us.
Over the last few months, we saw a slow decline in Sally’s health. It was mostly evident in seeing old pictures, and comparing now to how she looked and what she was able to do back then. She couldn’t walk well, she was walking on the outsides of her feet and had little stamina. Nicole and I were carrying her most of the time. She was falling a lot, and having more seizures. Mostly, it was becoming harder and harder for us to make her happy, to smile, which was taking both a mental and physical toll on our family.
About a month ago, Sally and Nicole were visiting our cousins when she had a high 104.7 fever, her heart racing. Nicole was up through the night caring for her to get the fever down. Like what often happened with Sally, these fevers would sometimes come and go, with no explanation. That happened here.
Over the span of 3 weeks, Sally was miserable. She was crying or upset almost non-stop. She kept telling us “I’m scary” which was her way of telling us she was scared. She kept telling us her tushy or stomach hurt. We couldn’t console her, and looking back we wonder if she was trying to tell us this was coming. We took her into the ER and they ran a ton of tests, including a urine sample. The tests all came back negative, there was thinking that she had a UTI, but the sample came back unclean. This despite us taking every step to secure a clean sample. This would happen with multiple samples over the course of the month. We were sent home thinking that the THC medical marijuana we had started her on may have been messing with her mind. We decided to start phasing it out, back to the CBD oil she was on previously. We saw some improvement, but not much.
This is around the time summer was ending. We managed to find a special swim vest online that allowed Sally to have some independence in the pool. She loved it. As a family we all got to take her into the pool and play with her. I did laps with her one afternoon, pushing her the whole way and she was so happy. We’re so thankful we ordered it, even though we only got to use it a handful of times.
Another joyous occasion occurred when Sally’s service-dog-in-training came home to us on Friday, September 7th. She was so happy when we brought him home, she even got him to sit for her the first night. Over the next few days she would walk Charlie from her stroller, holding his leash. If she was too tired, we’d hook the leash to the stroller just so she could participate. He’d even jump on her bed and stand over her in a protective stance. They slept in the same room, and both were happy.
Around this same time Nicole was bringing Sally to numerous MD appointments. Her school was closed, but she also didn’t have a nurse yet and couldn’t attend. None of the appointments yielded any answers for why Sally was spiraling downward. This caused great frustration for Nicole, seeing all these doctors and nobody could answer anything. At the same time, we were battling the Department of Education on securing busing for Sally. So many wasted hours and effort went into this, versus spending time with Sally those last few weeks. It’s a source of anger that we plan to address.
Although Sally’s birthday is September 11th, I took the 10th off from work since schools were closed and we decided to celebrate her birthday a day early. Sally asked for two things – to go out, and to eat lobster. She loved her lobster, and was one of the few foods she could eat, so we took her out to a restaurant. She was so happy to be out enjoying that lobster.
When we got home, we had some of her friends who live upstairs come down for some birthday whipped cream. She was so excited to introduce Charlie to them. “Come! Come! This is Charlie! Say hi to him!”. It was the most excited I’d seen her for quite some time. Sally had started to really enjoy the birthday song in recent months. She loved Frosty the Snowman and would often shout, “Happy birthday!” to us. She was thrilled to have us sing it to her, but my phone died in the middle of recording it and was lost. We decided to sing it again so we could re-record. Why not, it made her happy and she had earned the right to have it sung as many times as possible.
She was so happy that evening.
It was the last time we’d ever see her truly happy.
The next day on her actual birthday, we had to prep Sally for a endoscopy, bronchoscopy, sigmoidoscopy the next morning. This required her to fast and for us to do an enema for her that night. On Wednesday she underwent the procedures. Her GI track actually looked pretty good, Dr. Levy would stress this again in a follow up call he made to us this week. The pulmonologist saw some sign of an infection in her lungs, but they’d need to see what grew in the tissue cultures before treating it.

Charlie got into bed with Sally before she went to bed on her birthday and went into a protective stance.
On Friday night when putting Sally to bed, her heart rate was elevated. This usually indicated a fever was imminent, so we gave her Motrin and went to bed. The next morning she was tired. I got home from bringing William to his flag football game and Nicole was heading out the door to work. We noticed Sally was shivering. After Nicole left I took her in the bedroom and saw she had a 101 fever, so gave her Motrin. Her heart rate and fever would keep rising for the next two hours, it would finally subside in the afternoon. She was also urinating often, and asking to drink a lot of water, which was extremely unusual for her. We could barely get her to drink 3oz of water a day, she was drinking 20oz.

Sally walking Charlie Saturday morning, she was holding his leash but let go just before this picture. We realized she was fevering about 15 minutes later.
Sally and I sat at the table together that night and I fed her some food, she was hungry but not strong enough to feed herself. Nicole got home from work and I sat down and mentally relaxed for the first time that day. Minutes later Nicole realized that Sally was shivering again, sure enough the fever was still there. We put her to bed, only to be woken up starting at 3am continuously by her being uncomfortable and wanting to get up.
Starting at that 3am point, outside of a quick 60-min catnap one night, I would be awake for 68 hours straight. Nicole and I would be more stressed, more scared, and cry more than ever before over the next four days.
On Sunday Sally was uncomfortable, she had developed diarrhea and was continuing to ask to drink water, so much that we had to restrict her intake. She still had a fever, was not urinating and mostly laid in her bed or in her stroller. Our pediatrician told us to keep a close eye on her, and to give her a bit more time to see if she improved. I watched the first half of the Bills game and after hearing her discomfort decided to shut the game off, and just snuggle her. I took her into her bed, put on some shows, and we laid there together for three straight hours.
That was the last time I’d ever get to snuggle her.
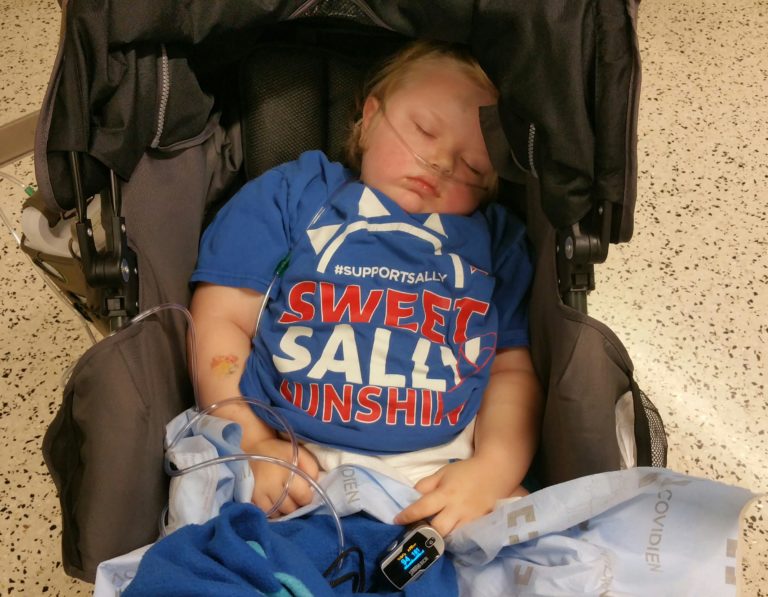
I took Charlie for a walk, and when I got back, Nicole told me she had thrown up. That was it for us. We often kept Sally home instead of taking her to the hospital as we were such experienced caregivers, and even the doctors acknowledged she was often better being cared for at home by us so as not to expose her weak system to infection at the hospital. They trusted us. However now we did not feel we could keep her hydrated, and needed to get some tests done to try and figure out what was brewing as we knew she was worsening. That was Sunday evening. We drove Sally to the hospital, something we’d done hundreds of times, but we didn’t know this would be the last time. On the way we noticed Sally’s oxygen needs increasing, she had been on minimal to no oxygen support for the last few weeks. There was traffic and I had to take all sorts of side roads to get us there.
The ER was ready for us, by now they knew Sally. Labs were quickly taken, she was sent for an X-ray. They knew Sally wasn’t right. For years Nicole had protected Sally’s veins, often battling nurses and doctors who thought they knew better. Her veins were extremely difficult to get an IV into, we’d always call in the best nurses or transport to do it.
We knew one day that we would need her veins, and said that every time somebody new went to stick her. This day turned out to be what we had saved them for.
A few hours later it was determined that Sally was experiencing severe sepsis from an unknown infection in her body. The ICU doctor I mentioned above came down to see us, to let us know he would be taking her into his care for the night. Sally’s standard WBC (White Blood Count) which indicates how your immune system is performing was around a 6.5. She had a really bad infection a few years ago where it jumped to 19, and it terrified us.
After the ICU doctor left, we learned Sally’s WBC was a 43, her body was fighting a severe infection.
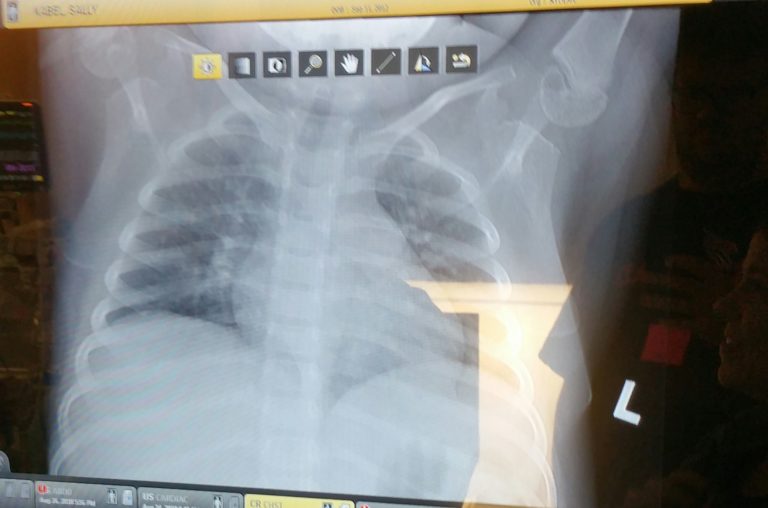
We got upstairs to the ICU, and the doctor showed us Sally’s X-ray from that night, versus one taken a few weeks ago. Unlike the previous X-ray you couldn’t see through her lungs to the other organs, which made him believe her lungs had collapsed. They started Sally on fluids and an antibiotic, switched her to a BiPAP machine so her lungs could be supported and we remained at her bedside as medical staff came rushing in and out. Around 5am Monday morning we decided I’d run home and get the boys to school. I got both off, did some quick shopping so they’d have what they need for a day or two, grabbed some supplies, then jumped on a bus into the city arriving back at 10:30am.
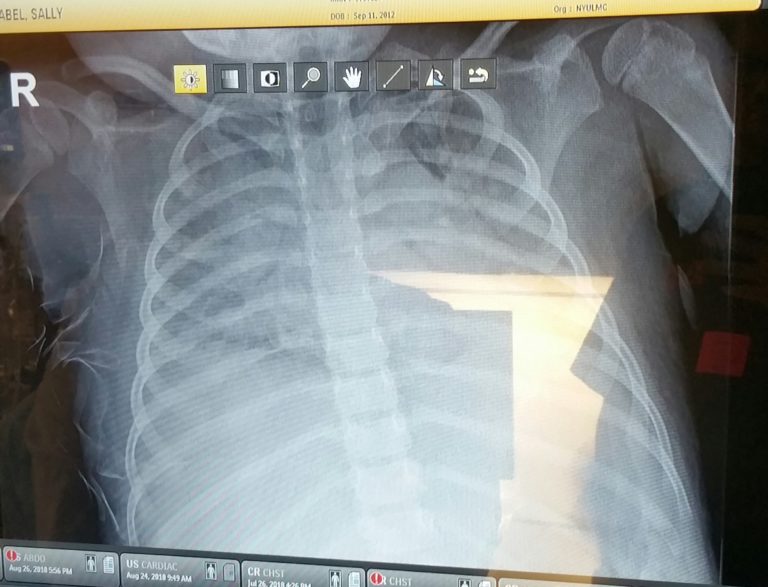
In the ER from that night, you can see how cloudy the space is now, which we learned later was fluid in her lungs.
Monday was a series of ups and downs, they struggled to get her stable. The fluids they were pumping into her were not leaving her body, she was still not urinating. Instead, she was retaining all of the fluids and blowing up like a balloon. This is something we saw happen at MSK numerous times. Nobody could ever explain why she always puffed up from IV fluids. We always avoided IV fluids for that reason, but we didn’t have a choice. A few doses of Lasix usually helped, but didn’t this time. Her nephrologist wanted to start her on dialysis to get the fluids off, but couldn’t until Sally was stabilized. Her blood pressure was low, so they put her on medications to constrict her veins to raise the blood pressure. This would come at a significant cost later.
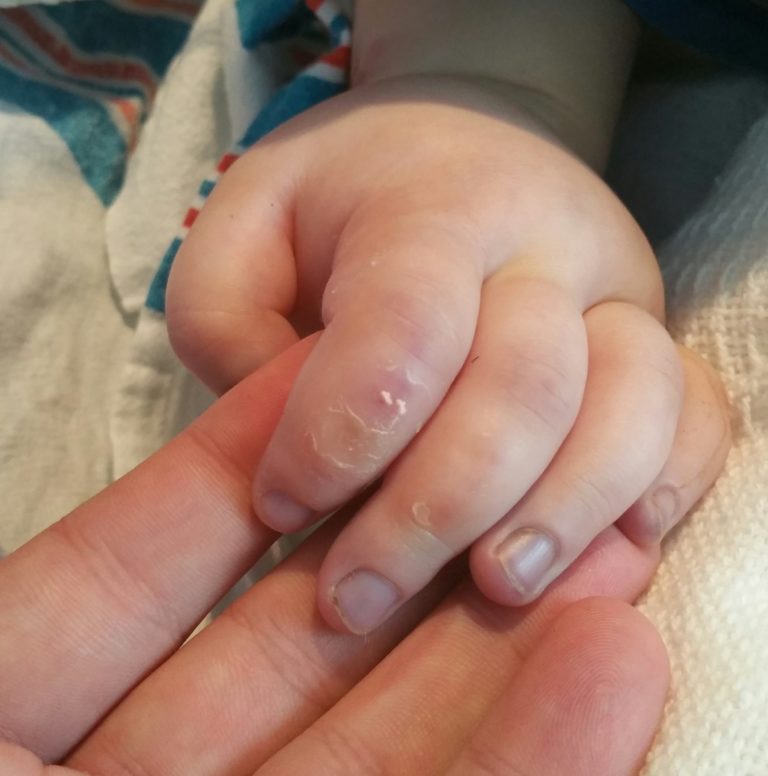
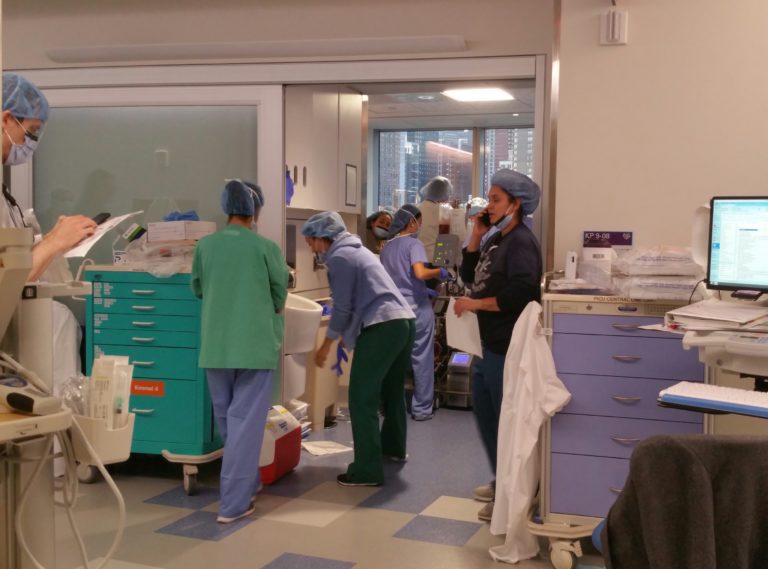
I took this photo, knowing I might not get another chance as the gravity of what was happening was starting to sink in.
While giving Sally some of her oral seizure med on Monday afternoon, her oxygen levels plummeted. The room was soon filled with nurses and doctors trying to revive her levels while Nicole and I watched in horror from the corner of the room. This is the point where we transitioned from being lead medical caregivers for Sally, to onlookers. This was new territory for us. We knew how to hospital, we’d done it so much over the last five years that we had it down to a science. Nobody could care for our girl better than us. Instead we were now on the sidelines watching helplessly, trying to stay out of everybody’s way.
After over an hour, they were finally able to stabilize Sally’s oxygen, but the decision was made to intubate her. The thinking was that if they could power her lungs and let them rest, doctors could work to stabilize her and let the antibiotics treat the infection. They moved the various machines around to create space and performed the procedure. Just before the procedure was the last time she was conscious. While inserting the tube, a ton of fluids came out of Sally’s lungs. Her lungs were filled with fluid, which explained what we saw in her X-rays the night before. She was now in septic shock, and they had found E. coli in her urine.
Nicole and I took a walk out to a peaceful dock by the water. We discussed the possibility that Sally might not pull through this, and had to start the discussion of what to do if it came to that. We decided that we’d have no regrets, that we knew we did everything we could and made the best decisions with the information we had. We shared our concerns and worries with each other, and ensured we were on the same page, knowing that this was likely going to get harder in the hours and days ahead. Team Kabel. We had not given up hope. Hope for the best, but plan for the worst is what we’ve always done. Nicole and I returned to the 9th floor and called our bosses, who are also our friends, and explained what was happening. We told them we needed to unplug and focus 100% on Sally. They understood, no questions asked, only offering love and support.
Even though Sally was sedated, the doctors said she could hear us. We decided to speak to her as much as we could and to play her music and shows for her. The nurses got their share of Angelina Ballerina, Curious George and Thomas & Friends episodes on an iPad by her head.
Sally struggled throughout the night, her room was filled with medical staff and loud machines. The nurses set us up on a couch in an empty patient room, I managed to get about an hour’s sleep before we had to leave so a patient could be brought it. Nicole would catnap when she could throughout our time there. We were stressed, scared, dehydrated and exhausted.
We returned to the couch in Sally’s room as we watched the staff struggle to keep her stable. By Tuesday morning it was clear that Sally may not survive. We also noticed that Sally’s fingers and feet were turning purple. It was from the medications used to raise her blood pressure. She was starting to lose her extremities from the poor blood flow to them. The staff decided to ease back on the meds causing it.
Nicole and I weren’t sure what do to with the boys. Do we have them come in, or should we have them remember their Sally before we came to the hospital should she not make it? We decided to call our friend Lou who had lost a child to cancer to get his advice on how to handle Thomas and William. He had literally texted me the night before to check on us. He said he didn’t have the solution, but talked us through the options. He made a comment that the boys are old enough to make their own decisions, and that if we took that decision away from them, they might have anger over it some day. Yes Lou, you did have the solution.
We decided to have the boys pulled out of school and brought in to see us. We took them into the playroom and explained what was happening. As always with them, we were transparent and honest. Thomas knew right away that the situation was bad and was upset. William, our little introvert, wasn’t as clear. To him, Sally always went into the hospital sick, and always came out. We gave them the option to go in and see their little sister, and had Child Life on hand to help us. We prepared them for all of the machines and that Sally didn’t look herself, that she wasn’t conscious. Each boy wanted to see her and went in one at a time to speak to her, the nurses and Child Life staff explained everything and coached them through it.
We all went downstairs and had lunch together. We saw our nephrologist who said Sally was stable enough and they were going to begin dialysis. She felt very confident that it would get the fluids off her and we’d see improvement in a few hours. Hope sank in.
After lunch we were engaged by the Palliative Care Team. In particular, one was a Nurse Practitioner that had transferred from Sloan Kettering and knew Sally. The other was coincidentally a pediatric oncologist there at NYU. The fact that one knew Sally and the other treated childhood cancer was one of the first of many signs we’d be sent in the coming hours and days. We had a frank and honest discussion about where Sally was at and where this could lead. They felt we made the right decision in how we handled the boys. We discussed what our baseline was with Sally, and what life we could we imagine for her. Essentially, what was the line in the sand between her living happily, and not.
We decided that our baseline was making Sally smile. If we could make her smile, we could work to overcome any other obstacles. This baseline would drive all decisions over the next 24 hours. They also told us that we’d potentially be hearing about a machine called ECMO, that carried significant risks, and that we needed to be prepared with that baseline should that conversation happen.
The conversation did happen. After the boys went home, we were engaged by the two ICU doctors on duty. One was the head doctor who brought us upstairs that first night, the other was a pregnant doctor who we really liked and had been Sally’s primary doctor so far this stay. They informed us that Sally had stabilized and they had begun dialysis, but it wasn’t working. Her blood pressure was just too weak. They could keep trying, but she would likely not survive. The last resort was a machine called ECMO. It’s mostly used in bi-pass surgeries, two large tubes are surgically installed in the arteries and the machine runs oxygenated blood into the heart, effectively running both the heart and lungs. They felt if they could do this, then Sally’s body could rest and be given time to heal. They also informed us that Sally was likely to lose part of her feet and hands due to the poor circulation.
For the machine to work, they could use an existing tube in her neck artery, but needed to insert a second hose into another artery near her neck, or her leg. If we chose her leg, they couldn’t guarantee it would have enough circulation, and she’d likely lose that leg. If we chose the neck, babies tolerate it well, but isn’t an option in adults as it causes massive strokes. Sally was in the middle of those two, and they honestly didn’t know what effect it’d have on her, but said some form of brain damage would be likely. We needed to make a decision, and fast. They left the room.
Death. Leg. Brain. Those were our options. Nicole and I spoke through it all, trying to overcome the emotional impact of each and look at it objectively.
Make her smile.
We chose to proceed with the ECMO machine, and to do it in her leg. Sally loved to dance, this would make it harder for her, but we’d do everything in our power to get her to dance again. Death was not an option at this point, and we felt her already compromised brain couldn’t endure any more damage with the neck option. If she survived but couldn’t smile or be happy, it would be selfish on our part.
At the same time, Sally became more unstable by the minute. Within minutes the staff had cleared out the room so that surgery could start in earnest. My sister Cindy, who had spent almost every single weekend helping us while Sally was on cancer treatment, had joined us and the three of us sat outside the room in chairs watching a room filled with surgeons work on our little girl, with a hallway filled with medical staff watching on.
At this same point, a rainbow appeared outside the window on what was stormy day. I commented out loud that it was a good omen, but in my heart I wondered if it was God telling us it was time for Sally to come home.

A rainbow in the distance. A friend would later tell us she saw the rainbow in Brooklyn, and it ended by Breezy Point, Sally’s happy place.
The procedure was supposed to take 45 minutes, but took twice that time. The doctors came out and told us the procedure was a success, but could only get about 80% of the flow required. They felt it should be enough, there was scar tissue in Sally’s leg that none of us knew about or how it had originated which made the procedure more difficult. The medical staff were relieved, Sally was on the machine and was stable. She had even urinated for the first time in days. Hugs were shared, smiles given, even some jokes made. The mood had lightened and Sally’s chances for survival went up a bit, the first time in days. We knew she was still critical, but there was hope.
I ran out to get us some food and came back to find Nicole asleep on a couch in the hallway. I went into Sally’s room and the head ICU doctor and I were alone with her. He felt good about the machine, and that she was stable. It was all in her hands now he said. He told me I looked exhausted, and I told him I’d been up for three days straight and was losing my balance in the bathroom. He replied that it was OK to go get some sleep, she was in good hands. The nurses arranged for us to have a room two doors down. We each took a couch and passed out from complete exhaustion.
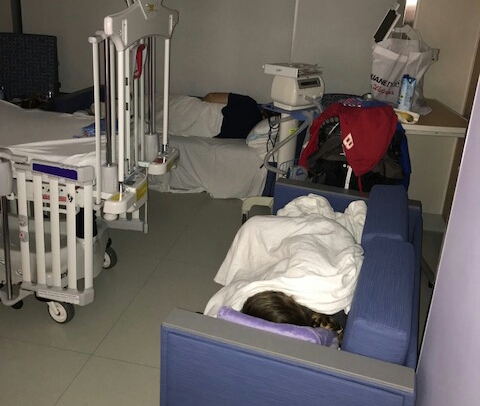
Our first real sleep in three days, looking back we wish we’d have slept less and spent more time in Sally’s room that night, but the nurses assured us they spoke and comforted her all night, even using their phones to play music for her.
Eight hours later we got up, Cindy had stayed up the entire night outside the room. She said Sally had a rough night. Nicole and I walked in to see Sally and I asked the usually upbeat nurse how our little girl was. Her hesitant and worried “Okaaaay” reply set off alarm bells immediately. A few steps more into the room and I understood. Sally’s body had retained all fluids, she looked like she was about to explode. everything was swollen, including her lips and ears. She was no longer stable and worsening.
We went back to the other room and the doctor came in to update us. The machine was not producing enough flow for Sally. It was an unforeseen complication and they were dealing with the manufacturer to see what could be done, if anything. She informed us that if they couldn’t get the machine to produce more flow, they had one final option. They could install a tube directly into her heart which would provide the flow they need. The surgeon was on his way up to evaluate Sally, and would be in shortly to discuss with us.
After an agonizing twenty minutes the surgeon came in and explained the procedure, but said he didn’t know if Sally could survive the surgery, let alone transporting her to the OR. He was willing to try it if we wanted, but said her chance for success was low. She could also need to remain secluded with her chest opened for days. A healthy person could endure it, he didn’t think Sally could, she was just too sick.
My brain was objectively evaluating the options, I hadn’t let emotion enter any decisions to this point. Make her smile. Nicole grabbed my hand and told me to follow her. She walked me into Sally’s room and we stood quietly next to her. I looked at my beautiful daughter and seeing her body in it’s current state, I broke down. I knew the decision we had to make, that I never wanted to make, was here. My sister had remarked that at one point in the night, Sally had tears and they thought she might be in pain. I shared that with Nicole and we knew we couldn’t do this to her any longer. Her body couldn’t take anymore pain. We decided that we had been away from her for too long, and would not leave her side again as we made our decision.
The head ICU doctor came in and the three of us sat down next to Sally. He again explained the surgeon’s views and shared his own, all options were gone and he did not feel she could survive. This confident doctor who felt so good about Sally’s chances a few hours ago was crying. He would keep trying if we wanted, all the way to the end, but didn’t think her body could take anymore. He asked if we could live with her passing away on an OR table away from us.
Nicole and I looked at each other and the decision was made, we embraced and cried. We did everything we could, the doctors did everything they could. They said we likely had a few hours, but Sally could leave us at any point. We decided to have the boys rushed in and that the four of us along with Cindy would be in the room with Sally at the end. Nicole went out to speak with the staff about what to do, and I sat with Sally alone.
I told her it was OK, she had fought so hard and we were so proud of her. She brought out the best in us and others. She had made us better parents, better people, better brothers, better spouses. She was the best daughter we ever could have had. It was OK to let go, she’d fought hard for too long. Mommy and Daddy love her, it was time to let go.
I sang ‘You are My Sunshine’ to her for the last time while she was alive. I’d never been able to say the “Don’t take my sunshine away” line to her, and had changed it to “You’re my sunshine each and every day”. This time, for the first time in five years, I used the correct words.
I went out and checked on Nicole, at this point the head ICU doctor was telling her it’d be better if the boys weren’t in the room at the end, based on his long experience with this. He said they should be given the opportunity to say goodbye, and then would leave the room. We could blame him for it. They could come in after to say their final goodbye. At the same time, we needed a priest, our friend Amanda had messaged me just before and offered to call one at her parish. We gave her the green light. Father Greg at our parish got the call, and agreed to jump in a car right away. The driveway was blocked by a parked car, the local police came and got him and rushed him in. I can’t tell you the relief we felt when he turned the corner and walked into the room, he had made it in time to perform the Anointing of the Sick.
At the same time the boys were just arriving. Nicole and I made quick preparations for how we wanted Sally to leave us. We quickly wrote up a list of her favorite songs from Maroon 5 to Thomas & Friends. The Child Life specialist downloaded the songs and gave us a speaker, Sally’s room would be filled with the music, just as she loved. Some of the nurses even danced and sang to Sally. They cleared out a room at the end the hall for close family an friends to come and sit with the boys when they arrived. We fixed up Sally’s bed by adding her blanket and we draped her shirt over her. We also put her doll next to her.
The boys arrived and were shown to the same playroom as the day prior. Nicole and I went in while Cindy stayed with Sally and Father Greg. We explained that we were out of options, and that Sally would be leaving us. Both boys broke down, they understood. We gave them the option to say goodbye. They both decided they wanted to, and we brought them each into the room so they could talk to their sister one last time. William asked to take a photo of her with his camera, we knew it was a way for him to process it so allowed him to do it. Somebody had turned down the music, to which he asked the staff to turn it back up because Sally loved her music.Thomas told Sally how much he loved her. Fr. Greg led us in prayer, we said the Our Father as a family. Fr. Greg left, we then asked our other close family and friends who were there to say their goodbyes. After everyone went, we knew it was time.
As the staff prepared the room by removing most of the machines and situating Sally so we could get into bed with her, a poster arrived from Sally’s school. It was made by the teachers and students, and had pictures of Sally with her friends and get well notes. I remember remarking “oh thank god, just in time”. The ICU staff didn’t know a healthy Sally, and kept asking what her baseline was. We were able to show the staff who Sally is. The social workers put tape on the poster and we all stood outside the room. The staff finished preparations and told us to quickly go inside. They could only make room for one parent in bed with Sally, Nicole and I looked at each other and I said it had to be her, she is the one who carried her into this world, spent almost every night with her in hospitals, had slept with her for two years of treatment and nursed her for 3+ years. She needed to be laying with her as she left us. I sat in a chair on the other side with my face next to hers and my arms wrapped around her. Cindy sat at the foot of the bed, present for Sally but giving us space. The poster of Sally’s photos was hung on the window next to us.
We told her how much we loved her, thanked her for being such an amazing daughter, for being the best gift we ever received. We told her we were proud of her, and it was time to let go. One day we’d see her again and be reunited.
They informed us that they were turning off the machines. It was instantaneous, her pain was gone, her fight was over, she was now in a better place where she could dance as much as she wanted and eat anything. The medical staff quietly cleared the room and left us with the sounds of Sally’s music playing and our tears.
Cindy left Nicole and I to be with Sally. Nicole and I cried over her, spoke and sang to her. The ICU doctor came in a little while later and placed his stethoscope on her heart.
“She’s gone.”
We decided that we’d get Sally dressed so everybody there could say goodbye, knowing we would not be doing a wake. The doctor removed the tube from Sally’s neck at our request, Nicole used gauze to keep the area clean to the surprise of the doctor while he worked. We had done so much medical care for Sally, this would be the last procedure and she’d help do it herself.
The nurses came in and together, the four of us bathed Sally and wiped her down. Nicole washed her hair. The pregnant ICU doctor who we really liked came in and while crying, helped Nicole put a dress on Sally. A blue dress, her favorite color. Sally loved her band-aids, and we used them to cover up anything from all of the tubes and IVs she had. Nicole brushed her hair one last time. We put her “baby” next to her along with the blood draw supplies our little nurse-in-the-making loved to play with. We turned the music up.
Again, we gave the boys the option to come in and see Sally, both of which accepted. Thomas went in and said his goodbyes. William came in and was scared, we directed him away to our family. Everyone else soon joined us in the room as we said our goodbyes. At the end, Nicole and I took a few lockets of Sally’s hair so we could keep a part of her. They have become our most cherished possessions. We also took a copy of Sally’s thumbprint to be made into a charm later.
As Nicole packed up I sat quietly with Sally, going over the six years we had with her. I sobbed. I also knew I needed to share her passing as I wanted to ensure her village heard it directly from us. They’d supported her all these years and deserved that, so with her next to me I posted to her pages through my tears the worst news we could share. The posts I never wanted to make in the five years of me making them.
Nicole saw the hospital’s music therapist outside, who Sally loved. She always loved music therapy. She asked if there was anything she could do, and Nicole asked if she would come in and sing some final songs to Sally. She knew exactly what Sally wanted to hear. As Nicole and I snuggled Sally one last time, she sang “Hello Sally”, “Sugar” and “You are My Sunshine” acoustically, it moved our hearts. It was beautiful, and we know something Sally would have wanted. We’re sure the therapist likely struggled to keep her composure, but she did up until the end of the last song.
It was time for us to leave, Nicole and I said our final goodbye after ensuring the nurses would not leave her side as we left, the two who helped us bath her for the final time. We can’t say enough about the compassion we experienced from the entire staff at NYU. The night doctor came in and asked to see her twice privately, emerging with tears both times, as did one of the Physician Assistants and other staff who were with her those four days. Our nurses were wonderful, they cared for Sally as if she was their own, even playing music for her and talking to her when we couldn’t be in the room. We have always loved nurses, they were our saviors those few days as always. In fact, nurses from the other floor who treated a healthier Sally came in to say goodbye. The way the hospital handled the whole situation was wonderful considering the circumstances.
We left the floor without Sally, I stopped and placed my hand on her door as we walked down the hallway, guilt and sadness that she wasn’t coming with us. Downstairs Nicole took the empty stroller, filled with our bags instead of our daughter, away from our niece who had been pushing it, and pushed it out the front entrance for the last time. It was a finality that she herself had to experience.
We told NYU that they needed to learn everything they could from Sally, anything that could help another child one day. We gave permission to do an autopsy, as in-depth as they needed. We know we’ll get the call that they’re ready to share results in about two months, we dread that day, and also know we may not get any answers. Sally always liked to keep doctors guessing. Due to the timing, we could only sign up for one study, and epilepsy focused one that will study her brain tissue. The only part of Sally we could donate was her corneas, and hope they found use for them.
We have been trying to process what transpired this last week. We went from going 1,000 MPH for five years, to a standstill. There is no Sally to give meds to, nobody calling out to us in the middle of the night, we don’t need two hours of prep to leave the house. Mornings are quiet and the hardest part of the day. There are no doctor appointments. We never thought we’d mourn the sound of those machines, but we do. We spent our first day without Sally down at Breezy Point, Sally’s happy place. At the beach we sat around her pictures, sang and shared our favorite Sally sayings before heading over to the cabana where she loved to play. We truly felt close to her spirit there, it was the one place she was always happy, and always wanted to go.
We had just received Charlie and were training him to be a service dog. Instead, he’s become a support for William and Thomas. We’ll continue his training to be a therapy dog instead, and hopefully take him to visit nursing homes, hospitals and special-needs kids. William has really embraced Charlie, so he’ll lead the effort with his little sister’s dog.
People have asked how they can help. We honestly don’t know, this is still raw to us. Our friends at Arms Wide Open started a fund for any unexpected medical or burial costs, therapy for the boys and any other needs. Any unused money we plan to donate to Sunrise Day Camp and Kids Need More, both are summer camps free and dedicated to local childhood cancer families like ours. They have been a huge support for Thomas and William, and will continue to be in the years to come. You can donate by clicking here, we asked that $1 be listed as the goal so nobody feels pressured to give unless they want to.
This Thursday at 7:45pm we are holding a candlelight vigil for Sally as Coney Island’s Parachute Jump lights gold for Childhood Cancer Awareness. On November 3rd at 2pm, we’ll hold a Memorial Mass for Sally at St. Patrick’s in Bay Ridge. Following the mass we’ll hold a Celebration of Life event celebrating Sally, a fun party with everything she loved. Sally loved her parties.
We had requested people wear gold or yellow last Friday after Sally passed. The response was overwhelming, our entire neighborhood is decked out in gold ribbons, yellow balloons, signs, paintings. We received an equal response of Sally’s village around the world wearing yellow for her and sharing photos with us. Here is an article on the Bay Ridge portion of it: Click Here
One thing we noticed was that in addition to all the yellow and gold, we saw sunflowers everywhere. They were placed on ribbons. They were painted on windows. We saw naturally growing ones all over the neighborhood. They were everywhere. We’d never really strongly associated Sally with the flower, but here they were screaming to us. They’re tall, they’re bright, they’re beautiful, they’re strong, a little wild, they follow the sun!
In speaking this out with Fr. Greg while we made Sally’s arrangements, he explained that the sunflowers were Sally, and she was telling us she was OK and in a better place. Whenever we see sunflowers, we’re to know it’s just our girl surrounding us with her love. As Fr. Greg asked, what do sunflowers do? They multiply and spread. Our fear is that Sally will be forgotten, we hope what she taught us continues to spread.
Please keep Sally and our family in your thoughts and prayers. We thank you all for the love and support you have shown us not only for the last week, but for the five years our little girl fought. We love you all.

On the day after Sally passed away, we all went out to the beach at Breezy Point, Sally’s happy place where we felt close to her.
Mommy & Daddy














I love you guys.
Thank you Matt for sharing Sally with us. We are all better for knowing her and she will remain with us always. It felt her while reading your beautiful words. Sending love always.
Love and hate this entry at the same time but want to share something with you about Friday when you had requested people to wear yellow for sweet Sally. We were traveling that day and had packed a yellow t-shirt for childhood cancer awareness that I had put on. During the travel that day we stopped to do photos in Yellow Springs Ohio and the purpose for this was that we wanted to take photos of the sunflowers. When I read this post it seemed like it was a reminder of how precious your daughter was and that she really was a sunflower during her brief life.
It is almost to hard to speak. Tears are clouding my eyes. I grew to love you daughter so. I feel I have lost a loved one. One I had prayed for, hoped for wished I could help. You, your beautiful daughter and fantastic family is unforgettable. I will always hold Sally in my heart and continue to pray for her. She will not be forgotten. I hope you will not forget us who have become part of your family. I wish you the best but know the sorrow you feel will never go away.
The poor soul suffered so much – all you did was the best anyone could do. You were brave, loving and compassionate. No regrets onlybwishes that could not be. Be safe, be healthy and continue to be the most amazing people I know. With sincere love.
My heart breaks for your entire family. Please know that your precious Sunflower girl will always be remembered by me! I have followed her story for years now and feel heartbroken to hear of her passing. The way your family has handled and shared your story with the world is truly remarkable and I thank you! So many life lessons to take away from Sally’s life and stories. You both were so fortunate to have that precious girl in your life and you both must be pretty incredible parents that God chose you both to be Sally’s parents! I pray for peace for your entire family and know that you all have made an impact on so many of us out there.
Words don’t seem adequate to express my sorrow at the passing of your beloved Sally. Your eloquence is unmatched. Thank you for sharing your story. Sally’s life and legacy will undoubtedly help so many who have to follow your path. God has given you strength to help others in the time of your greatest need. I pray that your family finds solace in the years to come. From the Irish proverb “May the road rise up to meet you, May the Wind always be at your back, and May God hold Sally in the palm of His Hand until you meet again.”
I am so sorry. I have read about Sally all of the years. I am deeply sad and sorry. She was certainly loved and will be with you forever in your heart and memories.
Matt & Nicole, Thomas & William, & Charlie,
The one blog I had hoped that I would never have to read, I am so sorry that little Sally has passed but I know now she is in a better place, with no pain. She meant a lot to so many of us who kept her and your family in our prayers. Having lost 2 children of my own, I can understand what you are and will be going through for many years to come. She was quite the fighter and went thru so much. Her little body finally wore out and couldn’t take it anymore. She was escorted to heaven by an army of angels. God Bless Sweet Sally Sunshine and all of you. You all will always be in my thoughts and prayers and thank you for allowing me and all of us in on Sally’s journey. Love to all of you, Dorothy
I have read each and every word of this story….with tears yet hope. My daughter, who is 32, was very ill at age 10 and nearly passed. she had been in a car accident. I will never forget this story and Sally, though we are strangers. Please keep us all informed as time passes, I want to know about how your family is doing! Your sons, your dog (adorable!) and mom and dad….I feel like I know you. The daughter I spoke of lives in upstate NY, we are in Michigan….Blessings to you. I’ll never forget! Be well.
My sincere condolences to you and your family. Life just isn’t fair, but as you mentioned “Sally is free to dance as much as she wants now”, “no more pain” Sweet Sally! Dance with the angels beautiful Sally! God Bless you and your family! No more pain baby girl 💗
So, so sorry. Heartbreaking. Fly High ^^^Sweet Sally Sunshine^^^ Fly Free!!!
Dear Sally Sunshine you fought so hard and you were so brave. Your smile lit up the room and you were loved and cherished by so many people. You taught us so much. You will be in our hearts forever. Rest in peace sweet Sally Sunshine. Your pain is gone and you are free to dance and do all the things that you loved. Keep smiling <3
Dear Matt, Nicole, Thomas and William and Charlie so sorry for you loss. No words to truly express. Please know that you are being lifted up in my prayers. Thank you for sharing Sally with us and your journey. May the Lord continue to watch over you all and bless you. With my deepest sympathies and much love. Daisy
I just read the entire blog-tears in my eyes. I have followed your blog on Sweet Sally all these years. I do remember seeing you and your beautiful family at the Surf Club. My heart is broken for all of you. Please know that you’re in my prayers and Sally will never be forgotten.
Matt & Nicole – there are no words that I can offer that will comfort you. Just know that you and the boys are loved by so many and thoughts of Sally will remain with us forever.
Aloha Nicole and the Kabel family💕, I am so sorry and sad for your loss. I only met Sally in the womb and have watched through your posts all these years. Thank you for sharing her with all of us. You are an amazingly strong family. Much love to you🌻🌻🌻🌈
I don’t have the words…….no words to make this any easier…..I am so sorry for your loss of Sally….my cousin is a pediatric onocology nurse in FLA and she was with Sally in thought and prayer also this past 5 years…..We pray for you and the boys now, as I know Sally is finally in peace with the heavenly Father. You were the best parents any little girl could have had….always ALWAYS there for her. We also pray more funds are given for more research for drugs for children..God bless your family,now and forever
Our tears could fill an ocean.
I can’t begin to truly understand what you’re going through, but as I sit here in the wee hours hiccuping with sobs and taking in your beautiful and heartbreaking post, I feel close to her once again. See, Sally is one of those kids a therapist gets to work with once or twice in a career…the kind of kid who nestles her way right into your heart and makes you love your job that much more….a kid you never forget…a kid who plants a seed…apparently a sunflower.
Thank you so much for allowing us to be with you on your journey and during those final moments.
Love & comfort to you all. 🌻
Gi
Through our friends Lindsay and Mike Rhoades, Kate’s parents, I have prayed for Sally and your family for years. I will continue to lift you in prayer. You are wonderful parents and you have a wonderful family. The only part of God’s plan that is clear in this is that she was yours and you were her’s. I will never forget Sweet Sally.
Our thoughts and prayers are with your family. We do not know you but know you through Kristen Wells. I cried as I read your letter. May God wrap his loving arms around your family.
I am a friend of Ashley Allison and have been praying for you as you walk this difficult road. Thank you for what you wrote, it is heart breaking but strangely comforting. I will continue to keep your family in my prayers.
Lucinda
Wow I am so overcome sobbing through the entire blog for a girl and a family I only met ever so briefly. I lost my 57 year old sister 1 1/2 years ago to ALL and was with her at the end and I know that pain of wanting to see them set free and yet not wanting to say goodbye. I dont know how you will every “get over” losing Sally….of course you wont…but I also know you will honor her life in every way possible and make her sunshine shine for us all. I will not be there tonight at the candlelight vigil as I am out of town but will make every effort to be at her memorial. Your family has shown incredible strength through all this adversity and you are all an example of how to love. Thank you for sharing Sally with me she will stay with my heart forever. God bless you all and I pray for you all every day.
Thank you for sharing this intimate time in your journey with Sally. I pray for you and your family. You are unbelievable parents and wonderful human beings that are doing the best you can, still.
Thank you for sharing your little girl with us. You will heal, because Sally is always with you. ❤️😇
Tears running down my face. Thank you for sharing your journey. I admire the strength your family has had for the last years. She had the best parents she could have had. May your family find peace that she is out of pain. Cancer is a horrible thing and I’m so happy you fight for this cause. Sally’s life has touched so many people. What a blessing she was.
Put that fear away immediately – Sally will NEVER be forgotten.
My heart hurts reading this and the tears won’t stop coming.
So many of your words and details of that night and your time with Sally take me right back to my final night with Simone, three years and 1 day before Sally.
My thoughts and prayers are with you as we have traveled this same road you’re going down for three years. Simone also had an older sibling (7 when we lost Sim) and children and how they process and express their grief are so hard, especially when you’re dealing with your own loss and pain too.
Sally was an inspiration and she and so many of our kids deserved so much more.
I know she is happy and dancing and healthy and surrounded by the most amazing little crew of children up above, my daughter included.
Thank you, Matt, for your generous sharing of Sally’s passing. The posts of your family’s journey have touched us through the years, and now our hearts break with yours. Please know that we will always look at sunflowers differently because we will be thinking of your beautiful, brave daughter. We hope to join you in your battle to raise awareness of the need for more funding for pediatric cancer. And we thank you, Nicole and your boys for being role models as warriors for those we love and care for. May God bless, help you heal and bring you comfort through your memories of Sweet Sally Sunshine.
My heart is broken. I had so hoped and prayed that the outcome would be different. After the loss of my own son I didn’t want to see another family lose a child to cancer. Every time I see a sunflower I promise to look up to Heaven and say HI to your Sweet Sally Sunshine.
Hugs from another bereaved mom who understands.
My sincerest condolences to you all. I just adored her sweet little face and was so very sad to hear that she passed. I know nothing will ease the pain but I hope you find some comfort in knowing that Sally touched many lives in such a positive way and that you guys have brought much needed awareness to childhood cancer. You guys are amazing parents and caretakers and have her so much love. You and the boys and your whole family have been in my thoughts and prayers all week and will continue to be.
“She brought out the best in us and others.” No truer words could ever be written. (((hugs)))
As difficult as I know this must have been for you to write….it was beautifully written and heart felt. I’m so sorry you’re family has to go through this horribly difficult time, and the loss of your beautiful little girl. Even though I didn’t know Sally personally – only through your pictures and words I always prayed for her…..I hoped like you did….but sometimes you just have to let go. Absolutely hate those 2 words 🙁 Sally is in Gods arms now – and one day you will be together again. It was so hard reading your last days and moments……Tears streamed down my face. We will NEVER EVER forget the Sally SUNSHINE you brought to our lives. I pray that some how with the grace of God you are able to get through the days one little step at a time……LOVE YOU ALL……..miss you always <3 Miss Sally <3
Thank you for sharing your strength with the world. The bravery of your entire family is inspiring. Sally is loved. She will always be remembered.
Hi Matt,
I never met Sally or the family but i have been following her journey off and on for about 4 years. I think the first memory i have of you guys was the Empire State building lightup campaign. Thank you for sharing those final moments that are so precious to you and your family. My heart breaks for you, Nicole and the family. Reading this was very hard as a parent. I don’t know what it is to lose a child but being a mother of two girls, I know that the pain would be unbearable. I am praying for you guys and I have asked for my praying friends to help me. My prayer is for our Father in heaven to grant you all peace, comfort and strength for as long as you will need it, during this time. There is no doubt that Sally is smiling and dancing in freedom, no more pain.
My name is Nicole, owner of Nicole’s Gift Creations. I love sunflowers and I love sunshine. I already feel connectected to you guys that way but also through mutual friends. I hope to meet you all one day, to give you hugs. It would be an honor for me to be able to contribute to Sally’s Celebration of Life in November. God bless you all.
My heart is breaking reading this post that I know you never thought you would have to write. I can’t stop crying…There are no words I can say that will make it easier. But Sweet Sally will never be forgotten! Know that. Her life touched so many people. And you are an incredible family and parents. Your strength and courage through these years has been inspiring. Sally is at peace now…and dancing with the angels. My sincerest condolences to your family. I am so sorry. Much Love. Kathy
My deepest condolences , my heart goes out to you and Nicole ,and the boys.. I followed your story and though I didn’t know Sally personally, I felt like I did. She was amazing.i remember when Nicole was pregnant! I worked at tlc had the pleasure of being Thomas and William teacher ! You and your f Family will be in my prayers . God bless you. Sleep in peace sweet Sally sunshine💛💛💛💛🌞🌞
Dear Cables, my heart goes out to you. You have bravely & lovingly cared for Sally from the day you learned of her illness. God be with you. I know your hearts are broken. You will be in my prayers.
Love,Ethnea Runfola
God is good…………………All the time!
Thank you Matt for sharing, with such love and devotion, Sally’s final days. She is at Peace and now surrounded by sunshine.
Much love from your Bills family in Portland Oregon.
Thank you for sharing your journey with the world, it puts a perspective and faces of real people on what it is like to live with illness. It filled my heart with sadness and love. I wish your entire family peace and love and sunflowers forever.
I have been following Sally’s journey for quite some time now through instagram. Although i did not personally know Sally or your family, I felt like I had some connection with her. When I read of her passing I immediately had tears in my eyes. This little girl was truly a fighter. My heart goes out to you guys and your entire family. Your little sunshine touched the lives of so many people she had never even met before. Reading about her journey each day and seeing updates when she was doing good, made me feel so happy. Happy that your little girl wouldn’t let her sickness defeat her. You guys are truly amazing parents. You stuck by her side, gave her the absolute best care she could ever get. She fought through til she just couldn’t anymore. I read this entire post and it was truly beautiful. Thank you for sharing these final moments of your little girl. She was peaceful in her mommy’s arms with daddy right there. No more pain for little Sally, she is now resting peacefully. She is a little angel now watching over you guys every day. Your little guardian angel. You are in my prayers.
Lots of love,
Mia
I am in tears reading this post, the photo of you holding her hand made me loose it all. My heart goes out to you, Matt and your family. I never got to meet Sweet Sally but I followed her story since day one and felt like she was family to me. You and Nicole are such an inspiration to many of us with your determination, love and strength, you both are outstanding parents. Sweet Sally will never be forgotten. Sending you and your family prayers and strength during this difficult time.
Sally was a joy to all who followed her. Our hearts are all broken for this loss. Thank you for sharing this beautiful sunshine ☀️ girl with us. Your family is in my prayers.🌻 🎗🌻
Im so sorry for your loss and pain. I used to live in Bay Ridge and remember you all well. I also used to be a child life specialist. My specialty was pediatric oncology and while reading this difficult post I found myself sobbing for all the little kids and families I had helped in this their most vulnerable and difficult time. I usually held it together for the families. I cried with many. This post had me balling. You have a long road ahead. Im happy to hear your dog will stay and help your boys. I loved providing pet therapy to the kids and families. You all are stronger than you know. Keep hugging each other. Allow your boys to mourn in their way. It doesnt ever really end. Let your community continue to support you. Sending you all lots of love, hugs and prayers from the west coast.
No words, just continuing to send hugs and prayers to you and your family. Matt and Nicole, you have inspired all who have come to know you and share Sally’s journey through the years. May you be comforted by her strength in the days ahead.
God bless.
I have no words. Just know we all are crying along with you and will continue to fight in Sally’s memory. Xo
My heart breaks for your family may god bless you always 😢
Prayers and Tears for Sweet Sally’s soul and you and all the Kabel family
We will continue to fight for all those so unjustly lost
I can’t imagine your heartache. I’ve been following Sally’s story the past 3 years. I cried with you multiple times reading this blog. May your boys, your wife and yourself be surrounded by love and light. Your family was nothing short of amazing (and still is). Thank you for sharing Sally with so many strangers.
Your family is in my prayers during this difficult time. Sally has been an inspiration to all of us following her story. She will never be forgotten!!
I lost my nephew to neuroblastoma at the age of 18 months. He too is a legand that will live on forever!! Please keep writing you and your wife are amazing thank you for sharing your story! 💛
This Sweet little Angel touched my heart…. she went home to be with Jesus on my Birthday…..my only Condolence was knowing that she is pain free, running, laughing, singing and dancing …then resting peacefully in the only arms that could possibly Love her more than her Earthly family….. the memory that popped into my newsfeed the next morning was of a Sunflower….and I too saw her Heavenly Rainbow the night before….a sign that Jesus was calling her home…..a Promise to Mommy, Daddy and Big Brothers ….. that she’ll be safe untill they meet again……all our Love to your family…… I’m so Happy that the Boys have Charlie too…..Prayers for strength…….
I am praying for your family . I have followed your posts and blogs about Your sweet beautiful little girl since you first starting posting them around the same time that a friend had said to me we need everyone to check and see if they are a match for sweet Sally sunshine she is such a beautiful Baby girl. She is terribly sick . Your daughter was taken way too soon and was a fighter as you know . She pushed through everything with her sweet loving personality never giving up . I am so deeply touched by your post as I read everything that happened . I felt connected to your family I felt such a strong powerful love coming out of your words . There are no words that I can find to exspress the deep condolences I wish to send to your beautiful family . Your beautiful daughter is dancing with the angels and I am sure she was embraced with a beautiful Gold shining world of love . As she went Home to our Lord . I will continue to pray for your family prays for your strength as you continue on . 🙏🏻🙏🏻🙏🏻
You words are painfully beautiful! Thank you for sharing this and Sally with us all! You are all in my prayers.
Words are so meaningless in times like these. I’m a complete stranger but I started following your baby’s story when I was pregnant with my
Daughter. Somehow your page kept coming up and I was drawn in by her sweetness. When I saw that she passed away I broke into tears, as if I had personally known her. She will never be forgotten, if she’s had this much of an impact on a complete stranger all the way across the country, there’s no way she will ever be forgotten. I know I will think of her and her fight and your family often. Wishing your family moments of peace that turn into hours and then days and weeks. I am so sorry.
Driving home from work today, I passed someone’s house and their entire front garden was full of sunflowers. I sadly smiled but thought of Sally. My heart has been broken for you guys since last week. I have thought of Sally every single day since then many times a day and know the world is a slightly darker place without her in it. I want to thank you Matt, Nicole, Thomas and William for sharing your sweet daughter and sister with us these past years. Watching her grow has truly been a gift. I cried reading this beautiful article wondering why this had to happen to such a precious angel. I know that God is taking care of her and while we’re all here crying, she is smiling without any fears or worries because she is safe and happy. I will forever think of sunflowers in a much different way and I will never forget Sally. The decision you had to make, Matt and Nicole was the hardest you’ll ever have to make, but you’re strength in letting her go so she can be free is more admirable than I can describe. There is a quote that I love, “When you can’t find the sunshine, be the sunshine.” Even if there were days where all there was were dark clouds and rain, Sally acted as her own sunshine and I can promise that everybody in this neighborhood will always remember the strength, courage, beauty, silliness, and bravery of your Sweet Sally. I am so sorry for the loss you are going to and will continue to pray for a four of you and also Sally. We all love you, Sweet Sally Sunshine, run and dance, and eat your lobster and always smile, you’ve certainly earned it.
This was beautiful Allie, thank you.
Thank you for sharing your daughter with us all these past years. Such a sweet little thing has taught so many about life. My heart breaks for you all. Continued prayers for her and your family. I know I’ll see your daughter’s beautiful smiling face in every sunflower I see.
My heart aches for you. I lost my 20 year old son to esophageal cancer.
Mat your memories of you beautiful Sally, making your heart smile, if only for a minute.
God Bless you all.
My heart and so truly aches as I read this, I cried a river of tears… I feel such pain for all of you and we hope you heal and find peace. Thank you for sharing her… we really do love her too…
🙁
Nellian and Family
I’m so sad for all of you, and Sweet Sally Sunshine! My heart breaks! It’s not fair!! 😭😭😭😢
I am so very sorry for your loss. I met your family when my daughter was at Memorial Sloan Kettering for surgery. My other daughter was very close to Sally’s age and even looked a little like her at the time. Regarding the sunflowers, check out Maria’s field of hope
Online. It is a sunflower field here in Cleveland for pediatric cancer. So so sad many sunflowers and they will even send packets of seeds for you to plant. Again I am so sorry for your loss 💛🙏🏻🎗 Prayers
Blessings and prayers for your family. God has called another angel home and he will take good care of her until you meet again. I am so sorry for your loss🙏❤️
I cried all the way through this but thank you so much for sharing. We all know your journey is far from over. Please consider continuing to write and keep us up to date with Thomas and William and your new service/therapy dog. We have all come to love you and your family.
Thank you for sharing your beautiful story of Sally. ❤️😥
My heart breaks for all of you. Thank you for sharing Sally with us. Love as peace to you and your family.
I have no words, only tears.. I didn’t know about your little girl until I come across this today but I can tell how much she is truly loved. We almost lost our little girl last year to a rare illness that attacked her spinal cord and as I lay here holding her and crying for your loss I want to say how sorry I am and how my heart breaks for you. I worry everyday just as you did and I wish more than anything that Sally was here with you still.. thank you for sharing your beautiful daughters story with us.. I will think of her always from what I read.. she seemed like a wonderful angel on earth and now one in heaven ❤️❤️❤️ Rest easy sweet Sally❤️