
William comforting Sally while she’s having a seizure at the table. The boys have learned to identify them and know to alert us if they see one.
Hi all – We’ve been getting asked how Sally is doing a lot, most often in passing whether it’s on the subway or while we’re running to the grocery store. The question is impossible to answer in a quick sentence, so we figured it was a good excuse to share an update.
NYU summed it up for us last week by saying Sally is still in fair condition, but trending towards good. Prior to that, she was on the poor/fair side of the scale. From where we were at six weeks ago when we were seeing sometimes 50 seizures a day, we’re now seeing fewer than half that and sometimes less depending on the day. The combined regiment of Onfi, Depakote and now the Modified Atkins Diet appear to have stopped Sally’s downward spiral and she’s been showing signs of improvement. We’ve also decided to keep her on cannabis for now so as not to make too many changes at once. Long story short, we’re trending in the right direction but still have to take it a day at a time.
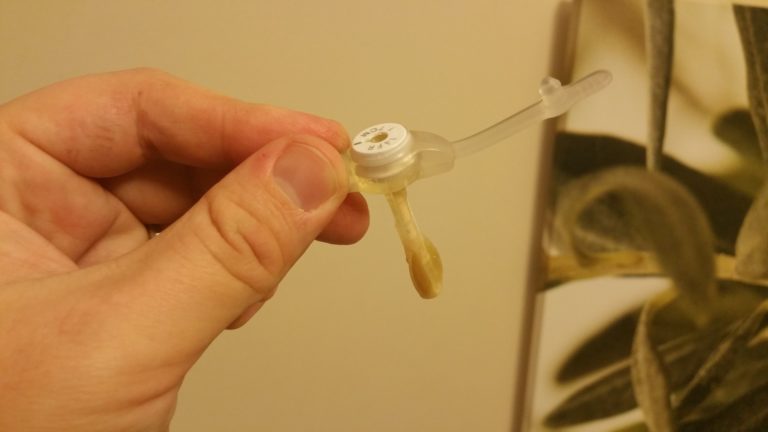
We started Sally on the Modified Atkins Diet at Dr. Devinsky’s team’s urging two weeks ago. In summary, the diet consists almost entirely of fat and a little protein. Everything is cooked/soaked in fat. The challenge is that Sally is only permitted 10 net carbs A DAY. To put that in perspective, the average apple has 20 net carbs! Keeping in mind that Sally has only been eating solids for just over a year, and doesn’t have the jaw strength to eat most meats, we knew this would be a challenge. Nicole has fired up the Kabel Test Kitchen, experimenting with different recipes we’re gathering. So far Sally’s favorite meals are eggs mixed with heavy cream cooked in ghee/butter, and a version of mac n’ cheese with riced cauliflower in place of pasta. She’s permitted a couple of berries during each meal, which we use as bribes to get her to eat everything else. In addition, we’re in the process of switching all of her meds over to pill forms that contain no sugar that we can crush and push through her feeding tube. This comes with challenges, the first vitamin we tried clogged Sally’s g-tube and we had to urgently switch it out of her stomach so she could get her seizure meds on time. It’s been a lot of trial and error, and Sally can often show her sass by refusing to eat, but we feel it’s already having a positive impact on her.
We reached out to our Nurse Practitioner on Dr. Devinsky’s team and asked that since Sally was no longer trending downward, if we could we take a step back and regroup. We’d never really had anybody walk us through and explain Sally’s seizure activity to us. She confirmed that the damage to Sally’s white brain matter, caused by the chemo, is directly leading to her experiencing Generalized Seizures in both sides of her brain. The three types of seizures Sally has (Absence, Myoclonic, Tonic) all fall under the Generalized diagnosis. All three are serious, but the tonics are especially so as they can cause extensive damage the longer each lasts. These were quickly getting out of control in the fall which is why Sally was admitted. Although we’re now seeing fewer, we still do see them. We’ve also learned that they can be triggered by stress, which we’ve learned the hard way. There’s few things that can make you feel worse than triggering a seizure for Sally, whether it’s by pushing her too much to use the potty or to eat her food. We’re learning to back off and try different approaches to minimize her stress. It can be a challenge when she’s refusing to take her seizure meds and you can’t delay them.
At the same time, Sally is experiencing frequent activity even when seizures aren’t occurring. This activity is a wave pattern on the EEG that shows her brain building up to a seizure, but not quite enough to trigger an actual seizure. In Sally’s case, this is occurring throughout the day and extensively through the night.
This activity is having an impact on Sally’s cognitive function and learning. During the day, the activity causes almost constant “interference” for Sally. It was described to us as if having a conversation with somebody while another person is hitting you in the arm constantly. The distraction/interference would make it impossible for you to absorb the conversation and everything around you. At night, this interference grows more intense. When your body sleeps, your brain is processing everything it learned during the day. With all the activity occurring, Sally is not processing what she’s learned at the level of other kids. Combined, this interference is causing impairment of Sally’s cognitive function and her ability to learn. She’s still young and her brain will continue to grow, so we need to work on addressing this for her long term benefit.

As much as Sally loves dancing, it’s clear she lags behind the other kids her age in class. It’s hard for her to keep up with them and to maintain her attention.
As a result, our priority outside of managing the seizures/interference is to secure a school that can work with this impairment. We’ve identified a private school that has been recommended to us which is equipped to handle a child with Sally’s challenges. We are currently working through the application process, and if accepted will require an arduous process for us to be able to afford sending her there. However, we know the limitations of public schools and know it would be the best situation for Sally’s long term growth to send her to this school.
Finally, Sally’s original EEG at Cornell showed a slow spike-and-wave pattern in line with Lennox-Gastaut Sydrome (LGS). This can lead to a very poor long term prognosis. Fortunately, NYU has not seen this pattern in Sally’s last two EEGs, which means the Onfi dose she’s on is currently working to treat it. This is something we didn’t have clarity on until last week and was a relief to hear. However, although Dr. Devinsky doesn’t feel the need to label her as having LGS, he wouldn’t disagree with another doctor who would diagose her with it since she has the right symptoms.
Right now we’re trending in an improved direction, our short term goal is to maintain the current drug regiment while continuing the Modified Atkins Diet to hopefully realize its full potential. Over the next few weeks we need to observe if Sally’s seizures are continuing to improve, and if school is seeing an improvement in her cognitive function and learning. In the near term we’re being cautiously optimistic, however are also taking it day to day and trying to prepare ourselves should she begin trending downward again. We know that the other post cancer treatment kids with seizures like Sally have not had long term success with the current drugs/diets/treatments available. As discussed with NYU, our long term plan is to keep Sally stable as long as possible while new treatments and drugs are being developed. Basically, we’re waiting for science to catch up with Sally.
Please keep Sally in your thoughts and prayers.
Matt & Nicole



Thank you for the update on Sally. She has a special place in my heart and is in my daily prayers. You are amazing parents and I pray that God will bless you and continue to give you the strength you need to provide Sally with the best of care. Your boys are great, too. Sincerely, Tina Bonitatis
As always, your precious Sally, and your whole family are in my thoughts and prayers.
Always in our prayers
My thoughts and prayers are with you and Sally everyday. Trending toward good is wonderful news.
Encouraging. Everyone is rooting for her.
I think of Sally often. And hope for her to do all that you hope her to do. She is so very lucky to have such smart parents who are doing everything under the sun to help their beautiful little girl. When I look at the Empire State Building I think of Sally and think of your families determination. Stay strong.
I think of Sally so often and each of you. Your courage and determination for finding the best is so beautiful and I truly pray that god answers all of your prayers. Your boys are so loving with their baby sister and while I’m sure you are so proud of them as a parent I know it breaks your heart to have them worry with this. May everyday be better and better and may Sally be fully healed and each of you
Thank you for the update. You are all in my prayers every night. So happy to hear that Sally is on an upswing. Hang in there knowing you have numerous people reaching out to you.
Thank you for these updates. I am always thinking about Sally and she is in my prayers. I so wish she wasn’t facing these long term effects of treatment. You continue to do the very best for her in every way – I am praying for you guys also for wisdom and strength in all of this. On, a lighter note – our eight year old Ruthie asked if Sally was wearing a Quidditch helmet(!) – this is a Harry Potter reference if you aren’t yet fans. She said this in an admiring way about the cool helmet. 🙂 I really do appreciate the updates, it is heartbreakingly helpful to hear what is going on with Sally.
Thank you for all the detail, Matt. You guys are amazing and it’s heartening to hear that medical knowledge and your constant attention to applying the strategies to guide her to health are working. ❤DK
Thank you for the update. I always include Sweet Sally in my prayers. May God Bless all of you for being such a great and strong family!!
Thank you for the update on Sally! I am glad she is in a fair condition and keeps moving forward. You are wonderful parents to always put Sally’s needs first. Prayers for Sally and your family!
Thank you for the update. Always in my heart…all of you ?????
Prayers & much love to our Sweet Sally!! From California Granny C & Papa L
Not a day goes by that I don’t look at Sally’s yellow bracelet and pray that God continues to give you and Nicole the strength and courage to support Sally and the boys.
If things ever calm down for you and Nicole, you should write a book on what to do, when to do it and all the recipes you have developed to help her.
Once Sally is accepted into the private school, you can apply to the Board of Education for tuition reimbursement. It’s a fight every year but they are required to provide the money needed to allow her to attend the school that meets her needs, since the public schools do not have the ability to do so.
Praying for such a special little girl & her family
Always Thinking of & Praying for Sally. Love to you all! xoxo
Praying that you continue in an upward direction. You are wonderful advocates for your child. God bless your family.
God Bless